Gastric Dilatation and Volvulus (GDV)
Gastric dilatation and volvulus is commonly called GDV and even more commonly referred to as bloat. The term bloat is somewhat of a misnomer because that really only describes half of the issue. This condition occurs when the stomach both dilates (fills with gas and/or fluid) and rotates on its axis. Unfortunately, we never know which happens first the rotation or the dilation. Regardless, surgery is necessary in order to correct the issue and prevent recurrence, we will describe the procedure below.
This condition most commonly occurs in the large/giant breed dogs and deep chested breeds. It is rarely seen in small and medium size breed dogs. The most common breeds are the Great Dane, Mastiff, etc – you get the picture. Surprisingly, in addition to the larger breed dogs, we also see it in Standard Poodles more frequently. There are a lot of theories out there as to why this may occurs. Some common thoughts range from frequency and size of meals, exercising after meals, elevation and height of bowls, etc. We also see an increase in GDV incidence in dogs that have other types of gastrointestinal disease, such as inflammatory bowel disease. Stressful environments such as pets being hospitalized, boarding, storms, etc. can increase the risk of this issue too. As a practicing surgeon, I can’t tell you how many times, dogs that present with a GDV are coming from a referring veterinary hospital, boarding facility, the pet-sitter, etc; so it is a real problem. A lot is done to avoid some of these situations to try to prevent this from occurring, the most definitive way to avoid this is to have a prophylactic gastropexy performed either by your veterinary or veterinary surgeon. I will address these techniques later on in the series, and we will spend some time on it, because this can be performed very easily by minimally invasive techniques.
Clinical Signs
Some of the most common signs an owner will see include the attempt to vomit, which is termed non-productive retching. This occurs due to the junction of the lower esophagus and stomach being rotated >180 degrees in effect kinking this area. Other signs are signs of discomfort such as listlessness and the inability to get comfortable. Also, many times you will notice enlargement of the abdomen. In cases that have been going on for some time (even a few hours) you can see dogs that are unable to get up and/or not responsive to stimuli.
As described above, this condition can progress rapidly and be fatal, so immediate veterinary care is a must. This condition not only directly affects the stomach and gastrointestinal system, but also affects the cardiovascular system (compression of the vena cava and return flow to the heart) which places these patients in shock and can propagate various inflammation and coagulation cascades that can also cause death. The spleen can also become affected due to its close proximity ad shared blood supply from the stomach. As the stomach rotates these splenic vessels can become torn.
Diagnosis
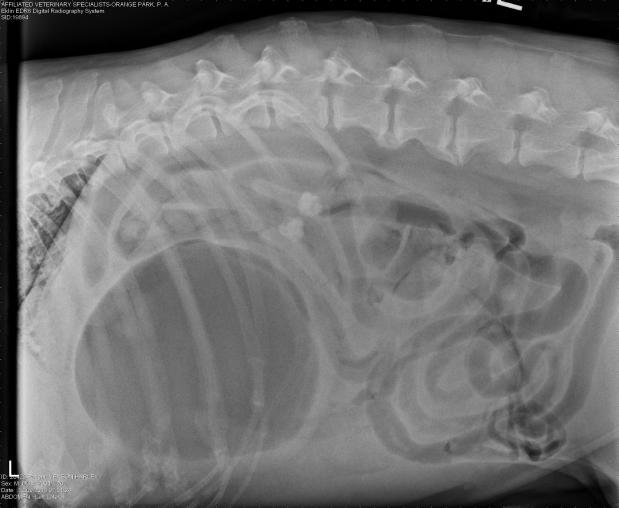
An experienced veterinarian will be able to quickly diagnose this condition, based on signalment (breed), clinical signs, and physical examination. Radiographs (X-rays) generally leave little doubt, as there are “tell-tale” signs seen on x-rays. Blood work will also be performed to assess values such as red blood cell concentration, electrolyte abnormalities, lactate, etc all factors that will be used to guide initial stabilization and treatment prior to surgery. Once diagnosed, surgery is required. If surgery is not feasible (patient is not able to be stabilized, owner unable to move forward with surgery, etc), humane euthanasia will be likely recommended.

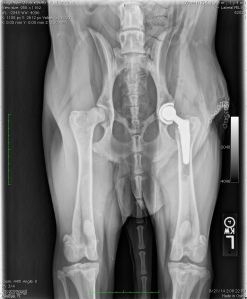
This is a right lateral abdominal x-ray. Note the large, dilated stomach and evidence of the duodenum (intestine) just above the stomach and below the spinal column.
Treatment
As one may assume anesthesia is more risky in a sick animal, but is needed for this problem. Unfortunately, there is no conservative/ non-surgical approach that has been shown to work. After immediate stabilization of the patient, surgery is indicated.
The surgical goals are to decompress the stomach, place the stomach in the correct position, and attach the stomach to the body wall – to drastically decrease the chance of this happening again. The last part of the procedure is called a gastropexy, dogs that do not have this performed, are at high risk for this to happen in the future.
Other things that need to be evaluated while in the abdomen are the stomach – there are times where necrotic (dying) segments of the stomach must be removed. Unfortunately, there are times where gastric (stomach) necrosis is so profound or is affecting a non-resectable location of the stomach when humane euthanasia may be recommended. Thorough evaluation of the spleen is necessary and a splenectomy may need to be performed. After these organs are evaluated, the rest of the abdomen is evaluated.
Post-operative care is also very important, since many cases are not completely straight forward. Close monitoring, aggressive fluid therapy and appropriate management is necessary for a successful outcome. More recent reports show an 80-85% survival rate (with straight forward cases), which is much higher than previously thought. The more damage done (gastric death, spleen involvement, etc), the worse the outlook. Again, a quick response and aggressive management is what is needed.
Prevention
While there are many different views about how to decrease the chance of a GDV occurring, the most successful way is to have a prophylactic gastropexy performed. A gastropexy is a procedure that attaches the pyloric antrum segment of the stomach to the body wall. While this does not prevent dilation of the stomach, it does prevent the deadly rotation of the stomach.
When is the best time to have this performed? I recommend this procedure be performed at 6 months or older. This timing of the procedure coincides with spaying and neutering of your pet, both procedures can be performed at the same sitting. This procedure is especially easy in female dogs that are being spayed, since the abdomen is already open.
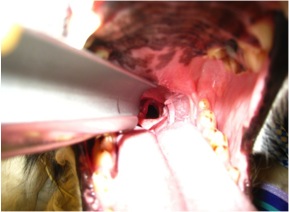
Recently, we have the advantage of doing this procedure and the spay procedure via laparoscopy. Laparoscopy is a minimally invasive procedure in which small incisions (0.5-1.0 cm) are made in the abdomen and the organs are visualized on a screen with cameras and surgery is done with small instruments through these incisions. The laparoscopic gastropexy is typically a very fast and effective procedure and is commonly combined with a laparoscopic ovariohysterectomy (spay). Contact your veterinarian for details about this procedure or a referral to a veterinary surgeon who can perform this procedure.